 These cells can be classified into totipotent stem cells, multipotent stem cells, and unipotent stem cells according to different differentiation potentials. A stem cell is a type of cell that is not highly differentiated and has the potential to regenerate various tissues, organs, and the human body. The administration of autologous bone marrow MSCs (BM–MSCs) to patients during the subacute phase of TBI resulted in improved neurological function in 40% of patients. To date, 125 clinical trials have been conducted using MSCs for neurological diseases, including TBI treatment. At the same time, the prospect of cellular therapy, represented by MSCs and exosome-based, cell-free therapy, is analyzed to demonstrate its therapeutic potential. In this review, we summarize the possible molecular or cellular mechanisms of MSCs as a therapeutic approach in TBI pathology. Taken together, this suggests that MSCs may be a promising cell-free therapy for TBI. Similarly, extracellular vesicles (EVs) released by MSCs cross the BBB and promote endogenous angiogenesis and neurogenesis, reduce inflammation, and facilitate cognitive and sensorimotor recovery after TBI. The latest studies have shown that mesenchymal stromal cells (MSCs) have great potential in treating TBIs due to their anti-inflammatory and antiapoptotic properties and the ability to generate new nerves. Pharmacological therapies reduce active bleeding, nourish the nerves, are anti-inflammatory, and include erythropoietin, tranexamic acid, and recombinant interleukin-1 receptor antagonist. Surgical therapies remove most of the skull bone by debridement decompression to reduce intracranial pressure and remove hematomas. Three main options are commonly used to treat TBI: hypothermic therapies reduce intracranial pressure, decrease inflammatory responses, and lower cerebral metabolic rate. Over the past few decades, treatment for TBI has always been a focus of attention. Therefore, new treatments for TBI can be developed by elucidating brain tissue remodeling and internal repair processes. The adult brain undergoes limited remodeling to compensate for tissue damage after TBI. However, inflammatory cells, such as neutrophils, are recruited to accelerate the inflammatory response and cause damage to peripheral tissues. The activation of microglia and astrocytes leads to the removal of cellular debris, restoration of the BBB, and production of neurotrophic factors. TBI may disrupt the blood–brain barrier (BBB) to cause neurochemical, metabolic, and cellular changes and activate microglia and astrocytes. The secondary injury is a progressive process that lasts from hours to days, which means that therapeutic interventions can be administered at this stage to avoid progressive nerve cell death and enhance functional recovery after brain trauma. The secondary injury is characterized by diffuse axonal injury and inflammation that can protect tissues from pathogens and remove cell debris however, severe cases can lead to neurodegeneration and secondary neuron death. 
The primary injury results from direct mechanical injury. TBI refers to the physical damage to brain tissue caused by a violent blow to the head. Severe TBI can trigger a long-term neurodegenerative process leading to pathological features and clinical manifestations similar to those of neurodegenerative diseases such as AD, structural destruction of neurons and functional impairment, and memory and cognitive decline, which in turn affect speech and motor systems. 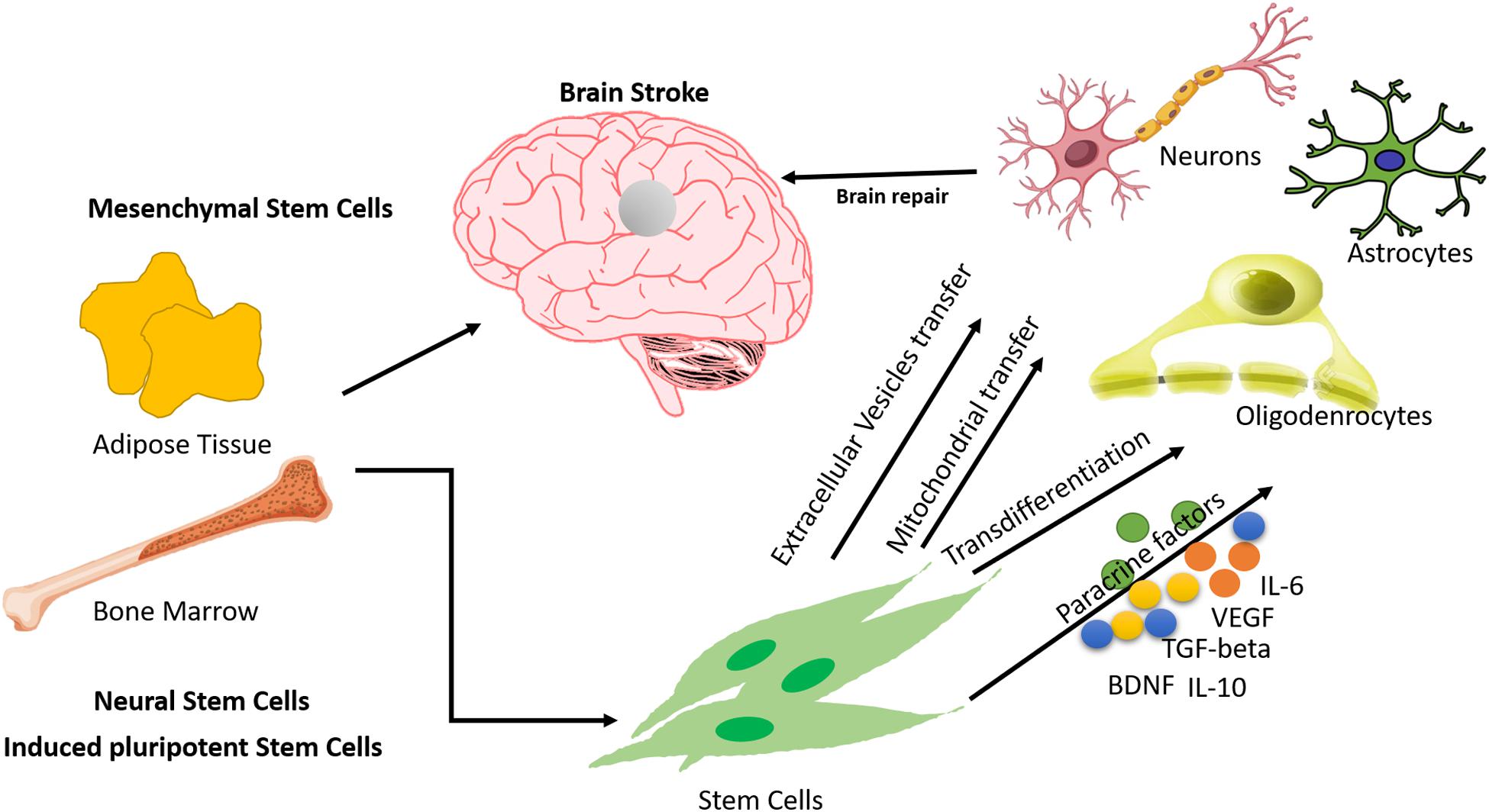
It has also been shown that TBI is associated with an increased incidence of common neurodegenerative diseases such as Alzheimer’s disease (AD) and Parkinson’s disease. More than 50 million people worldwide suffer from traumatic brain injury (TBI) annually, creating a significant burden on society and families. We also discuss research progress in the field of MSC therapy in TBI as well as major shortcomings and the great potential shown. In this review, we discuss the main pathological processes of TBI and summarize the underlying mechanisms of MSC-based TBI treatment. Recently, mesenchymal stromal cell- (MSC-) based therapy has shown significant therapeutic potential to target TBI-induced pathological processes, such as oxidative stress, neuroinflammation, apoptosis, and mitochondrial dysfunction. Its complicated etiology and pathogenesis mainly include primary injury and secondary injury over time, which can cause cognitive deficits, physical disabilities, mood changes, and impaired verbal communication. 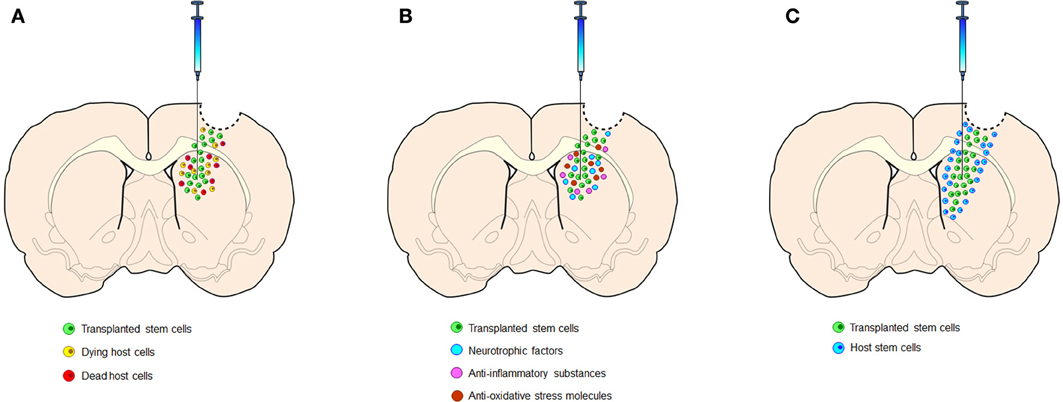
Traumatic brain injury (TBI) makes up a large proportion of acute brain injuries and is a major cause of disability globally. 
0 Comments
Leave a Reply. |



 RSS Feed
RSS Feed
